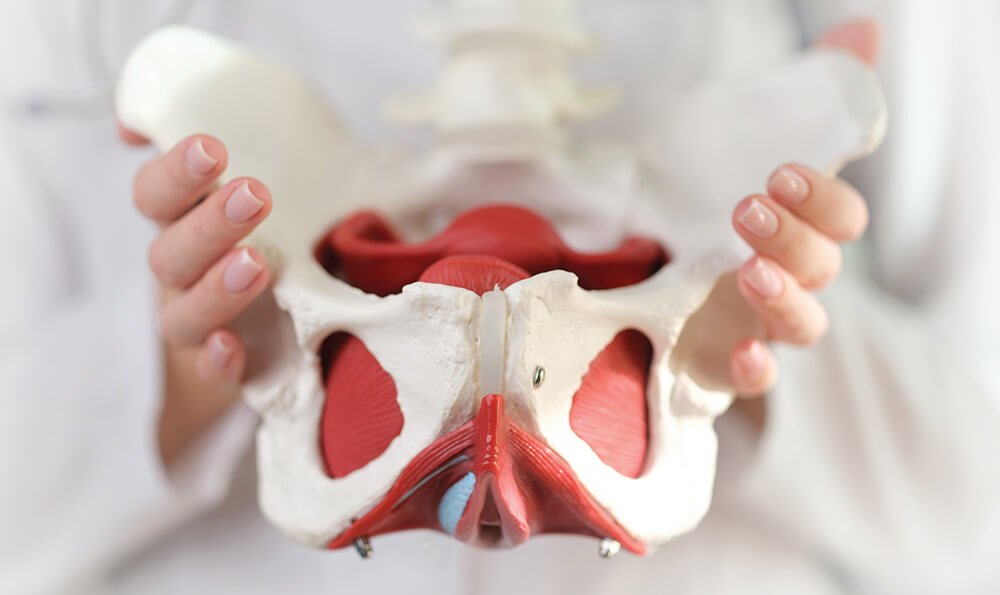
What is Pelvic Rehabilitation
Pelvic rehabilitation, also known as pelvic physiotherapy or pelvic floor rehabilitation, is a specialized area of physical therapy focused on the assessment and treatment of conditions related to the pelvic region. This includes the pelvic floor muscles, which support the pelvic organs (bladder, uterus, and rectum) and play a crucial role in bowel, bladder, and sexual function. Pelvic rehabilitation aims to address dysfunction and improve function in this area, promoting overall pelvic health and well-being.
The primary goal of geriatric physiotherapy consultation is to optimize the health, mobility, and quality of life of older adults, enabling them to maintain independence
The pelvic floor muscles can be affected by various factors, including pregnancy and childbirth, surgery, aging, hormonal changes, trauma, chronic constipation, and pelvic pain conditions. Dysfunction in these muscles can lead to a range of symptoms, including urinary incontinence, fecal incontinence, pelvic organ prolapse, pelvic pain, sexual dysfunction, and bowel dysfunction.
Pelvic rehabilitation begins with a thorough assessment conducted by a specially trained physical therapist. This assessment may include a detailed history, subjective interview, and physical examination to evaluate pelvic floor muscle function, strength, coordination, and flexibility. Assessment tools such as biofeedback, electromyography (EMG), and internal pelvic floor muscle examination may be used to provide objective data and guide treatment planning.
Based on the assessment findings, a personalized treatment plan is developed to address the individual’s specific needs and goals. Treatment may include a combination of techniques aimed at improving pelvic floor muscle function, reducing symptoms, and enhancing overall pelvic health. These techniques may include:
- Pelvic floor muscle exercises: Also known as Kegel exercises, these involve contracting and relaxing the pelvic floor muscles to improve strength, endurance, and coordination.
- Biofeedback: This technique involves using sensors to provide visual or auditory feedback on pelvic floor muscle activity, helping individuals learn to better control and coordinate muscle contractions.
- Manual therapy: Hands-on techniques such as soft tissue mobilization, myofascial release, and trigger point therapy may be used to address muscle tension, tightness, or trigger points in the pelvic region.
- Education and lifestyle modifications: Providing information on bladder and bowel habits, proper toileting techniques, posture, and ergonomics can help improve pelvic health and reduce symptoms.
- Behavioral strategies: Techniques such as bladder training, bowel retraining, and pelvic floor relaxation exercises may be used to address symptoms of urinary and fecal incontinence, urgency, and frequency.
- Relaxation techniques: Incorporating techniques such as diaphragmatic breathing, mindfulness, and relaxation exercises can help reduce pelvic floor muscle tension and promote relaxation.
- Functional training: Exercises and activities aimed at improving functional tasks such as lifting, bending, and carrying can help individuals better manage daily activities without exacerbating pelvic floor dysfunction.
Pelvic rehabilitation is a holistic approach that addresses the physical, emotional, and social aspects of pelvic health. By providing individualized care and empowering individuals with knowledge and skills to manage their symptoms, pelvic rehabilitation aims to improve quality of life, restore function, and promote overall pelvic wellness. It is important to seek care from a qualified pelvic health physical therapist who has specialized training and experience in this area to ensure safe and effective treatment.
